The
Echocardiogram
(Introduction << Previous
Page)
7/31/2008 |
|
The
echocardiogram was performed at a local heart center. It
looked like a sophisticated version of the ultrasound
that was performed on expectant mothers - but with doppler
imaging so parameters such as blood flow
aspects can be determined.
I
was able to watch the echo during the whole procedure.
The inside of the heart, the valve movement, etc, was all
clearly visible. Not knowing what to look for, I would
have no idea whether there was anything wrong. The procedure
was performed by an echo technician - who was apparently
not allowed to
answer questions
that
could an
any way be construed as a diagnosis. It was pretty facinating
overall to be able to have such a detailed real-time view
of the
heart pumping.
After
the procedure, I was sent to a waiting room, while the
Cardiologist interpreted the echo. I was not concerned
about what the the doctor had to say, because although
I was experiencing symptoms, I was never really sure whether
they were related
to my
heart.
Finally,
the Cardiologist walked into the room. After the initial
greetings, he asked me why I came in in the first place.
This seemed to be a positive question - as if he didn't
know why I should be there. I simply told him that I went
in for a routine Dr. Appt with my primary care physician
and he said I had a heart murmur, which should be investgated
further. Finally the Cardiologist said "You definately have some
things going on here". My 'heart' sank. Part of me
was shocked and scared - to have a Cardiologist (a title
in itself
that instills fear) say that I definately
had some things going on with my heart. The other part
was not suprised and even validated in that I could always
sense something wasn't quite right.
He
went on to ask me if I was experiencing symptoms, such
as shortness of breath at rest, swelling of the ankles,
etc. I told him I wasn't sure. I was never really sure
if the tiredness or fatique I was experiencing was a symptom
or normal. The only definative symptom I could identify
was the ocassional heart palpatations.
He
said that regardless of whether I was experiencing symptoms
or not, there were three main aspects of my heart function
that needed to be discussed. The three aspects, along with
their diagnosis were:
- Mitral
Valve Prolapse (moderate to severe)
- Mitral
Valve Regurgitation (moderate to severe)
- Left
Ventrical Dialation (4.6 cm)
Here
is an animation clip of the acutal echocardiogram, showing
the prolapsing valve. The animation is paused at the prolapse
so that it can be clearly seen.
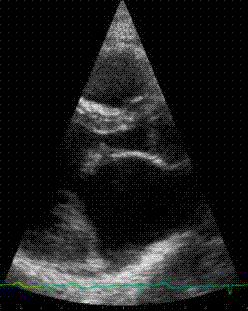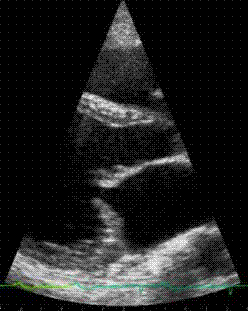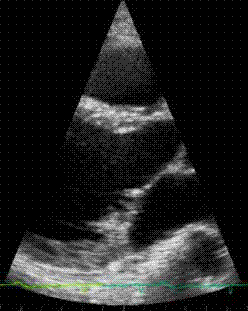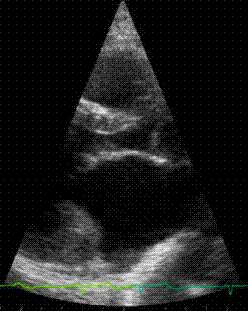
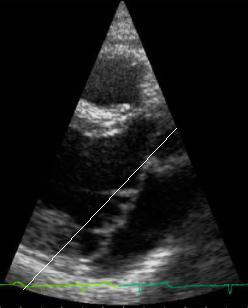
Click here for a larger, slow motion version The
image below captures the frame where the prolapse can most
clearly be seen. There is a line superimposed
over the approximate point where (according to the Cardiologists)
the valve should be stopping during a normal closure if
it
wasn't
prolapsing.
In other
words, the two leaflets shouldn't go to the right of the
line:
As
if the first statement by the Cardiologist wasn't enough,
when I asked him what needed to be done, he said that surgery
is the only option. Wow. I said "what kind of surgery?".
He said "Open heart is the only way to resolve this problem
- you will need surgery in no less than 10 years". This
was quite a shock. I went from feeling very healthy for
the
most
part,
to
apparently needing
open-heart surgery.
Next
Page >> Duke Cardiology
If this story has helped you, please donate. If took many hours to compile this information and costs time and money to maintain and update. Any donation is greatly appreciated!!
|
|